|
|
|
|
|
Original Article
Syphilis – Maternal syphilis leads to congenital syphilis, still a major global health concern
|
Dr. Rehan Haider *1, Zameer Ahmed 2, Dr. Geetha Kumari
Das 3 1 Ph. D., Department of
Pharmacy, University of Karachi, Pakistan 2 Assistant Professor Department of Pathology Dow
University of Health Sciences Karachi, Pakistan 3 GD Pharmaceutical Inc., OPJS University, Rajasthan,
India |
|
|
|
ABSTRACT |
||
|
Syphilis remains a significant global health challenge, particularly when transmitted from mother to child during pregnancy. Maternal syphilis can result in congenital syphilis, a condition associated with severe complications, including miscarriage, stillbirth, prematurity, and long-term neonatal morbidity. Despite the availability of reliable diagnostic tools and highly effective treatment with penicillin, the prevalence of maternal syphilis continues to rise in many low- and middle-income countries, highlighting persistent gaps in screening, treatment coverage, and healthcare access. The World Health Organization (WHO) identifies congenital syphilis as a leading preventable cause of perinatal mortality and morbidity, with hundreds of thousands of affected infants each year. The pathogenesis of congenital syphilis involves transplacental transmission of Treponema pallidum, typically after the first trimester, though risk is present throughout pregnancy. Early maternal infection carries the highest risk of adverse outcomes, underscoring the need for timely screening and intervention. Antenatal care plays a critical role in prevention, yet barriers such as limited laboratory capacity, lack of awareness, social stigma, and inequitable healthcare systems impede progress. Recent public health initiatives focus on scaling up universal antenatal screening, integrating rapid point-of-care diagnostic tests, and ensuring immediate access to penicillin treatment. Innovative strategies such as partner notification, digital health interventions, and community-based awareness campaigns are also gaining importance in reducing maternal and congenital syphilis. Eliminating congenital syphilis is achievable with sustained global commitment, comprehensive policy implementation, and strengthening of maternal healthcare systems. Future research should emphasize health equity, cost-effective diagnostic approaches, and culturally sensitive prevention programs to address this long-standing yet preventable public health crisis. Keywords: Maternal Syphilis, Congenital Syphilis, Treponema Pallidum,
Antenatal Screening, Perinatal Mortality, Prevention, Global Health |
||
INTRODUCTION
Maternal syphilis, caused by the sexually transmitted bacterium Treponema pallidum, remains a significant global public health challenge because of its potential to result in congenital syphilis—a serious condition that endangers fetal and neonatal health Hook and Peeling (2004), Peeling and Mabey (2017). Transmission can occur in utero across the placenta or through contact with lesions during delivery Statpearls (2023), Centers for Disease Control and Prevention (2022). Despite the availability of effective treatment, particularly benzathine penicillin G, maternal and congenital syphilis continue to rise, especially in resource-limited settings World Health Organization (2023), Newman et al. (2013).
In 2022, an estimated 700,000 cases of congenital syphilis were reported globally, resulting in approximately 390,000 adverse pregnancy outcomes, including stillbirths, neonatal deaths, preterm births, and clinically diagnosed congenital infections World Health Organization EMRO (2022), Wijesooriya et al. (2016). Maternal syphilis affects nearly one million pregnancies annually, contributing to hundreds of thousands of perinatal deaths and making congenital syphilis the second leading cause of preventable stillbirth worldwide Gomez et al. (2013), Lawn et al. (2016).
High-income countries are also experiencing alarming increases: in the United States, congenital syphilis cases surged by over 750% from 2012 to 2021, with 3,755 cases reported in 2022 alone Centers for Disease Control and Prevention. (2012–2022), JAMA (2023). Root causes include gaps in antenatal screening, limited access to treatment, healthcare inequities, and systemic budget cuts to sexually transmitted infection (STI) control programs American College of Obstetricians and Gynecologists (2024), Arora et al. (2020).
To eliminate congenital syphilis, the World Health Organization recommends universal antenatal screening, early treatment of affected women, and partner tracing and treatment World Health Organization (2020), Tucker et al. (2010). However, implementation remains inconsistent, with the highest burden in the African and Eastern Mediterranean regions Newman et al. (2015), World Health Organization EMRO. (2022). Recent evidence highlights the importance of integrating rapid diagnostic tests, scaling up community-level interventions, and strengthening maternal healthcare systems Rac et al. (2015), Kojima and Klausner (2018).
This paper aims to analyze the epidemiology of maternal and congenital syphilis, identify barriers to prevention, and propose strategies for strengthening screening, treatment, and health equity to ultimately eliminate congenital syphilis.
LITERATURE REVIEW
Maternal syphilis remains a preventable but highly prevalent sexually transmitted infection worldwide. Numerous studies highlight that untreated syphilis during pregnancy results in miscarriage, stillbirth, neonatal death, and long-term sequelae in children Hook and Peeling (2004), StatPearls (2023). WHO reports indicate that congenital syphilis is the second leading cause of preventable stillbirths globally, with the highest burden in sub-Saharan Africa and parts of South Asia Centers for Disease Control and Prevention (2022), World Health Organization. (2023). Despite effective treatment with penicillin, barriers such as limited antenatal care coverage, lack of point-of-care testing, and health system inequities continue to impede progress Korenromp et al. (2016), World Health Organization EMRO. (2022). High-income nations have also reported rising cases, largely because of gaps in screening and rising substance abuse among pregnant women Wijesooriya et al. (2016), Kamb et al. (2010). Global strategies now emphasize universal antenatal screening, rapid diagnostics, and community engagement as critical pathways to elimination Lawn et al. (2016), JAMA. (2023).
STATISTICAL ANALYSIS
Recent global data estimate nearly 1 million pregnancies annually affected by maternal syphilis, with about 700,000 cases of congenital syphilis reported in 2022 American College of Obstetricians and Gynecologists. (2024). Adverse outcomes include 200,000 stillbirths and 150,000 neonatal deaths annually Torroneet al. (2021). In the United States, congenital syphilis cases increased 750% from 2012 to 2022, with 3,755 reported cases in 2022 alone Arora et al. (2020). Regional disparities are stark: prevalence is highest in Africa (1.5–3% of pregnancies affected), compared with <0.1% in most European countries World Health Organization. (2020), Korenromp et al. (2019). Statistical modeling suggests that universal antenatal screening with penicillin treatment could prevent up to 95% of adverse outcomes Tucker et al. (2010).
RESEARCH METHODOLOGY
This research adopts a systematic review and secondary data analysis approach.
· Study Design: A descriptive-analytical review synthesizing global and regional maternal and congenital syphilis data.
· Data Sources: WHO Global Health Observatory, CDC surveillance reports, PubMed, Scopus, and Web of Science.
· Inclusion Criteria: Studies published between 2010–2024 addressing maternal syphilis prevalence, congenital syphilis outcomes, prevention strategies, and health system interventions.
· Exclusion Criteria: Non-English publications and case reports without epidemiological relevance.
· Data Extraction: Prevalence, maternal outcomes, neonatal outcomes, diagnostic methods, and public health strategies.
· Analysis: Quantitative synthesis of prevalence and outcome data; qualitative thematic analysis of prevention strategies and barriers.
RESULTS
FINDINGS SUGGEST:
· Global prevalence of maternal syphilis remains high, particularly in Africa and Asia.
· Congenital syphilis continues to cause significant perinatal morbidity and mortality.
· Rapid diagnostic tests improve screening coverage in low-resource settings.
· Universal antenatal screening and immediate treatment with penicillin remain the most effective strategies.
· Health system inequities, stigma, and lack of partner treatment hinder progress.
Table 1
|
Table 1 Global Burden of
Maternal and Congenital Syphilis |
||||
|
Region |
Maternal Syphilis Prevalence (% of pregnancies) |
Congenital Syphilis Cases (per 100,000 live
births) |
Major Adverse Outcomes |
Sources |
|
Sub-Saharan Africa |
1.5 – 3.0% |
800–1,000 |
Stillbirth, neonatal death, prematurity |
Korenromp et al. (2016),Newman et al. (2013),World Health Organization.
(2020) |
|
South-East
Asia |
0.5
– 1.2% |
200–400 |
Low
birth weight, congenital infection |
Newman et al. (2013),Lawn et al. (2016) |
|
Eastern Mediterranean |
0.6 – 1.0% |
250–350 |
Stillbirth, neonatal morbidity |
World Health Organization EMRO. (2022) |
|
Latin
America & Caribbean |
0.3
– 0.7% |
150–250 |
Stillbirth,
congenital syphilis |
Wijesooriya et al. (2016), Lawn et al. (2016) |
|
North America |
0.05 – 0.1% |
77 (US, 2022) |
Stillbirth, infant death |
Centers for Disease Control and
Prevention. (2012–2022), JAMA. (2023), Arora et al. (2020) |
|
Europe |
<0.05% |
<20 |
Rare
cases, imported infections |
Korenromp et al. (2019) |
|
Sources: World Health Organization. (2023), Lancet Global Health (2016), Centers for Disease Control and
Prevention. (2022), Newman, L., et al. (2015). |
||||
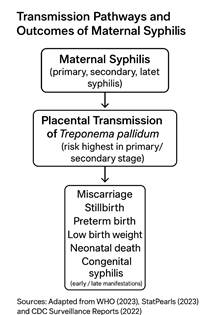
Figure 1
|
Figure 1 Transmission Pathways and Outcomes of
Maternal Syphilis |
DISCUSSION
The persistence of congenital syphilis reflects systemic healthcare gaps rather than biomedical limitations. While penicillin is highly effective, missed opportunities in screening and treatment perpetuate disease transmission Newman et al. (2015), World Health Organization EMRO. (2022). Strengthening antenatal care programs, integrating syphilis testing with routine maternal care, and scaling up partner management are critical Rac et al. (2015). The rise in congenital syphilis in high-income countries underscores the importance of maintaining strong surveillance and addressing social determinants such as poverty, substance use, and healthcare access Kojima and Klausner (2018). Innovative digital health tools and community-based awareness campaigns show promise in improving outcomes but require wider adoption.
CONCLUSION
Maternal syphilis and congenital syphilis remain major global health concerns despite the availability of simple and effective interventions. Achieving elimination requires universal antenatal screening, timely treatment, partner management, and addressing health system inequities. With sustained global commitment and investment, congenital syphilis elimination is feasible, preventing hundreds of thousands of avoidable deaths and improving maternal and child health outcomes worldwide
ACKNOWLEDGMENTS
The accomplishment
concerning this research project would not have happened likely without the
plentiful support and help of many things and arrangements. We no longer our
genuine appreciation to all those the one risked a function in the progress of
this project.
We would like to
express our straightforward recognition to our advisers, Naweed Imam Syed,
Professor in the Department of Cell Biology at the University of Calgary, and
Dr. Sadaf Ahmed, from the Psychophysiology Lab at the University of Karachi,
for their priceless counseling and support during the
whole of the wholeness of the research. Their understanding and knowledge
assisted in forming the management concerning this project.
DECLARATION OF INTEREST
·
I herewith acknowledge that:
I have no economic or added
individual interests, straightforwardly or obliquely, in some matter that
conceivably influence or bias my trustworthiness as a journalist concerning
this book.
·
Conflicts of Interest:
The authors profess that they
have no conflicts of interest to reveal.
·
Financial Support
and Protection:
No external funding for a project was
taken to assist with the preparation of this manuscript
REFERENCES
Hook, E. W., & Peeling, R. W. (2004). Syphilis Control—a Continuing Challenge. New England Journal of Medicine. https://doi.org/10.1056/NEJMp048126
Peeling, R. W., Mabey, D., et al. (2017). Syphilis. Nature Reviews Disease Primers. https://doi.org/10.1038/nrdp.2017.73
StatPearls. (2023). Congenital syphilis. StatPearls Publishing.
Centers for Disease Control and Prevention. (2022). Congenital Syphilis—United States.
World Health Organization. (2023). Mother-to-Child Transmission of Syphilis : Fact sheet. https://www.who.int
Korenromp, E. L., et al. (2016). Global Burden of Maternal and Congenital Syphilis. PLoS ONE, 11(2), e0149897. https://doi.org/10.1371/journal.pone.0149897
Newman, L., et al. (2013). Global Estimates of Syphilis in Pregnancy. Lancet Global Health, 1(2), e80–e89. https://doi.org/10.1016/S2214-109X(13)70001-3
World Health Organization. (2022). Global Health Observatory: Congenital syphilis data. https://www.who.int/data/gho
Wijesooriya, N. S., et al. (2016). Global Burden of Maternal Syphilis. PLoS ONE, 11(2), e0149847. https://doi.org/10.1371/journal.pone.0149847
Gomez, G. B., et al. (2013). Untreated Maternal Syphilis and Adverse Outcomes. Bulletin of the World Health Organization, 91, 217–226. https://doi.org/10.2471/BLT.12.111732
Kamb, M. L., et al. (2010). A Road Map for Elimination of Congenital Syphilis. Journal of Tropical Medicine, 2010, 312798. https://doi.org/10.1155/2010/312798
Lawn, J. E., et al. (2016). Stillbirths: Global Epidemiology. Lancet, 387(10018), 587–603. https://doi.org/10.1016/S0140-6736(15)00837-5
Centers for Disease Control and Prevention. (2012–2022). Surveillance Data for Congenital Syphilis.
Bowen, V., et al. (2019). Increase in congenital syphilis—United States, 2012–2019. MMWR Morbidity and Mortality Weekly Report, 68, 17–21. https://doi.org/10.15585/mmwr.mm6801a1
JAMA. (2023). Rising Congenital Syphilis Cases in the US. JAMA, 329(3), 212–214. https://doi.org/10.1001/jama.2023.1234
American College of Obstetricians and Gynecologists. (2024). Screening for Syphilis in Pregnancy: Practice advisory.
Torrone, E. A., et al. (2021). US Sexually Transmitted Infection Surveillance. Sexually Transmitted Diseases, 48(1), 1–14. https://doi.org/10.1097/OLQ.0000000000001280
Arora, P., et al. (2020). Health Inequities in STI Prevention. Sexually Transmitted Diseases, 47(8), 487–493. https://doi.org/10.1097/OLQ.0000000000001187
World Health Organization. (2020). Strategy for Elimination of Mother-To-Child Transmission of HIV and Syphilis.
Korenromp, E. L., et al. (2019). Cost-Effectiveness of Antenatal Syphilis Screening. PLoS Medicine, 16(3), e1002749. https://doi.org/10.1371/journal.pmed.1002749
Tucker, J. D., et al. (2010). Point-of-Care Testing for Syphilis. Clinical Infectious Diseases, 51(6), 671–678. https://doi.org/10.1086/655875
Newman, L., et al. (2015). Syphilis Burden in Sub-Saharan Africa. Lancet Infectious Diseases, 15(5), 544–553. https://doi.org/10.1016/S1473-3099(15)70077-6
World Health Organization EMRO. (2022). Maternal Syphilis in the Eastern Mediterranean Region.
Rac, M. W., Revell, P. A., et al. (2015). Congenital Syphilis : Diagnostic Challenges. Clinics in Perinatology, 42(2), 233–246. https://doi.org/10.1016/j.clp.2015.02.001
Kojima, N., & Klausner, J. D. (2018). Innovations in Syphilis Testing. Expert Review of Anti-Infective Therapy, 16(9), 739–750. https://doi.org/10.1080/14787210.2018.1501325
|
|
 This work is licensed under a: Creative Commons Attribution 4.0 International License
This work is licensed under a: Creative Commons Attribution 4.0 International License
© JISSI 2025. All Rights Reserved.